19A121
CASE OF ATYPICAL CUTANEOUS MYCOBACTERIUM CHELONAE INFECTION IN PATIENT OF SYSTEMIC LUPUS ERYTHEMATOSIS AFTER CYCLOPHOSPHAMIDE THERAPY.
Author(s)
Dr Sheraz Rasool, Dr Amr Afifi, Dr Denise De Lord.
Department(s)/Institutions
Department of Internal Medicine & Rheumatology, Queen Elizabeth the Queen Mother Hospital, East Kent University Hospital, Margate, Kent, UK.
Introduction
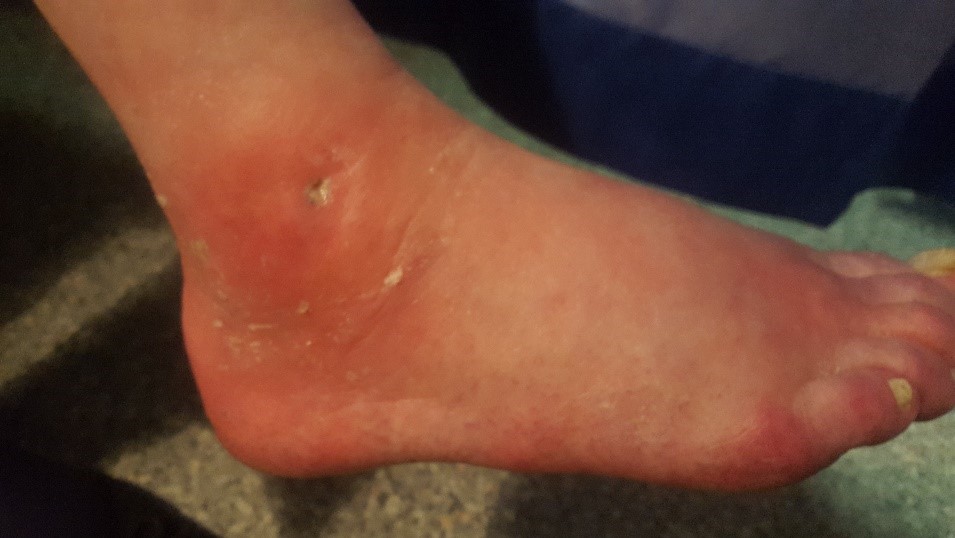
Mycobacterium Chelonae is one of the rapidly growing non-tuberculous mycobacteria that can be isolated from water, soils and aerosols. Localized infections have been reported associated with tattoo parlors, pedicures and cosmetic procedures. But disseminated infection is usually associated with individuals who are immunocompromised, predominantly affecting limbs but sparing abdomen and back. We herein present a case where patient was on immunosuppressive therapy and developed locally severe infection around right ankle.
Aims/Background
Mycobacterium chelonae is known as a non-tuberculous environmental mycobacterium, belonging to the M. fortuitum complex, acid-fast bacilli, non-pigmented and with a fast rate of growth; it was first isolated from a sea turtle named Chelona corticata, but it is usually found in the water, soil, dust and contaminated instruments. There are multiple reports of this infection after trauma, surgical procedures and other procedures including acupunctures, pedicures, subcutaneous injections, pacemaker implants. It can cause both soft tissue and skeletal infections in healthy individuals but disseminated infection usually occurs only in immunosuppressed patients. Clinical manifestation can vary from local abscess or ulcer formation to multi organ involvement. Diagnosis is confirmed by taking biopsy sample of affected tissue, Ziehl-Neelsen staining, histopathological examination, molecular biology methods, culture in appropriate mediums and RNA probes. These non-tuberculous mycobacteria are resistant to conventional anti tuberculous drugs and there is no randomized controlled study to suggest particular therapy for these infections, however four to six months of clarithromycin has been prescribed successfully previously with very few cases of resistance.
Method
first acute flare of Lupus, Second atypical Infection post chemotherapy involving skin and muscles. Third was Malignancy
Results
She was admitted for triple regimen as per microbiologist guidelines. She was started on Intravenous tobramycin, imipenem and clarithromycin. Non-tuberculous mycobacteria are resistant to conventional antituberculous drugs. Likely course of treatment will be at least six to twelve months depending upon response to therapy
Conclusions
• Locally aggressive infection or disseminated disease warrants treatment from 6 to 12 months as per drugs susceptibilities.
• Best medications to consider for M. Chelonae are Tobramycin, Imipenem, Clarithromycin, Linezolid, co-trimoxazole.
• Multiorgan involvement is must to be ruled out, as it can cause mortality if it disseminates and involve lungs particularly