19A124
Disseminated Pnuemococcal Infection in an Immunocompromised Rheumatic Disease Patient
Author(s)
Kieran Murray, Anna O'Rourke, Candice Low, Eoin Feeney, Eric Heffernan, Douglas J Veale
Department(s)/Institutions
Saint Vincent's University Hospital
Introduction
An 88-year-old woman with RA on adalimumab presented to the Emergency Department unwell for three weeks. Initial symptoms were fatigue, jaw and elbow pain. She was commenced on oral ibuprofen and prednisolone by her GP for a suspected RA flare but failed to improve. In the four days prior to hospital presentation, she developed fevers, headaches, vomiting, rigors and somnolence.
On admission, she was febrile with meningism, confusion, global weakness and a tense warm left elbow effusion. She had elevated neutrophils (18.6 x109L) and C-reactive protein (364 mg/L). Left elbow X-ray was suggestive of an olecranon bursitis. CT brain with contrast revealed a right infratemporal fossa fluid collection extending into the right temporomandibular joint (TMJ) and a left cerebellar lesion consistent with an abscess. CSF showed 13 white cells per cmm (99% polymorphs), red cell count of 8 per cmm, protein 3.27g/L (normal 0.15-0.45) and glucose 0.1mmol/L. Cefotaxime, vancomycin, dexamethasone and intravenous fluids were commenced. Adalimumab and prednisolone were discontinued.
Aims/Background
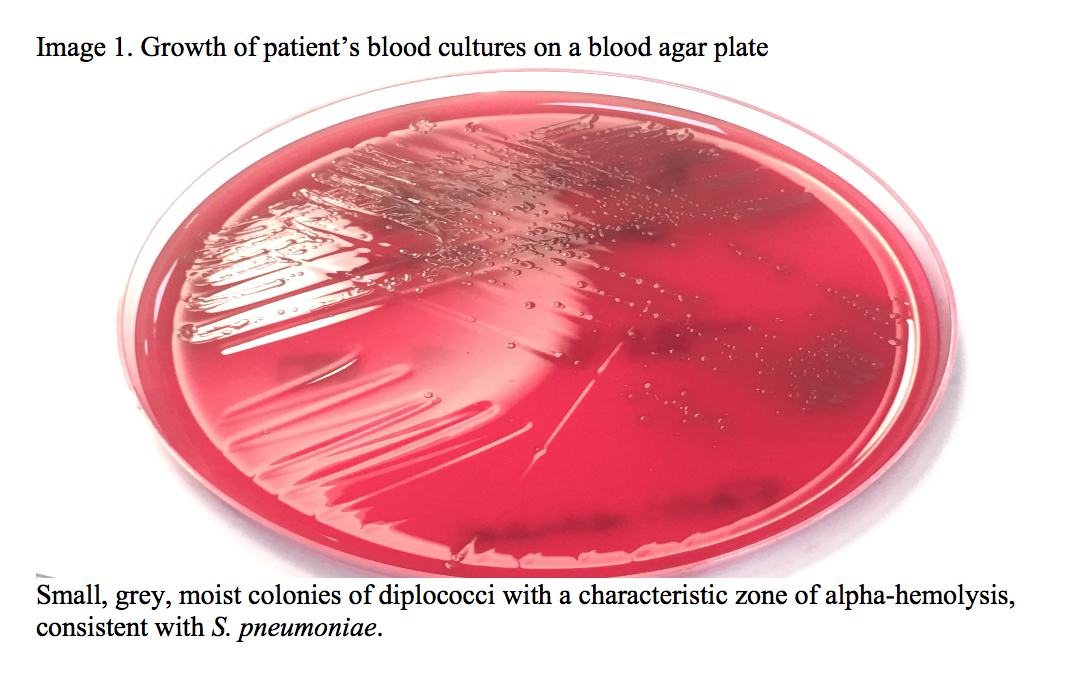
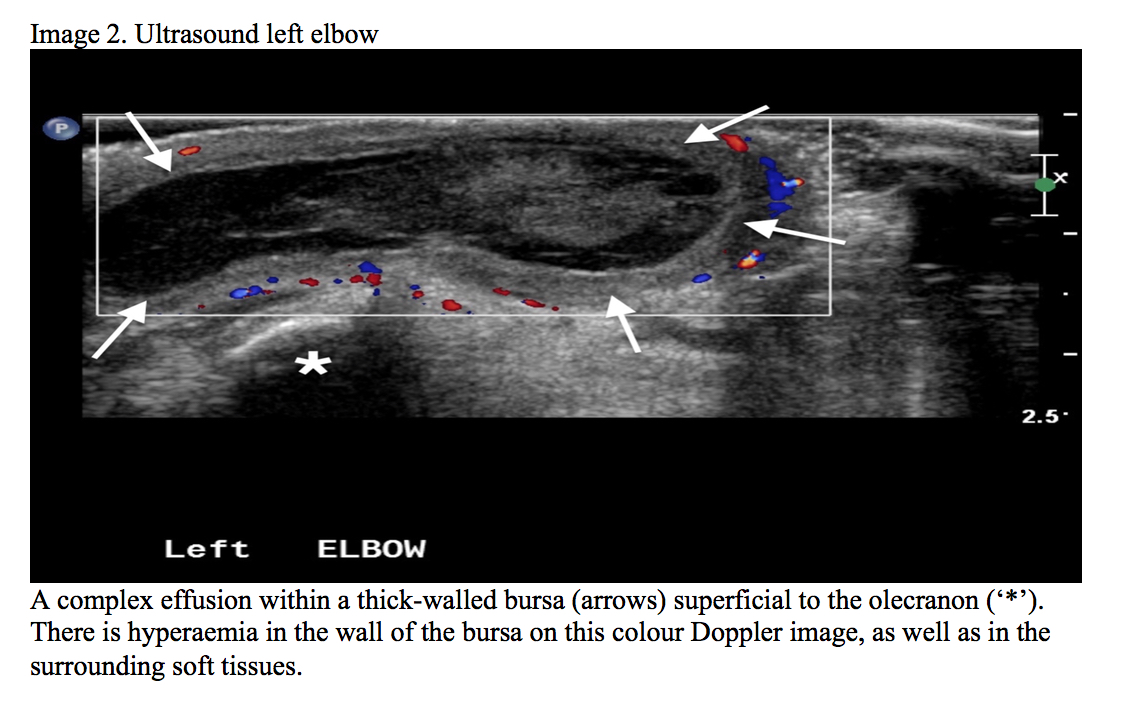
Pneumococcal urinary antigen was positive. CSF and left olecranon bursa aspirates showed gram positive cocci. Streptococcus pneumoniae was cultured from blood (Image 1), CSF and left olecranon bursa cultures. The patient had never received pneumococcal vaccination. Ultrasound showed effusions superficial to the left olecranon (Image 2) and in the TMJ. MRI brain showed a hyperintense rim enhancing fluid collection extending around the right neck of the mandible.
Method
The patient was treated with IV cefotaxime and had three drainages of her olecranon bursitis. Otolaryngology and maxillofacial surgery advised conservative treatment of her TMJ effusion and abscess.
Results
After 28 days IV cefotaxime, she was transitioned to oral amoxicillin and discharged to community rehabilitation. She made a full recovery and remains off immunosuppression.
Conclusions
This patient had a life-threatening case of disseminated pneumococcal infection with an infected olecranon bursitis, meningitis, TMJ effusion, left cerebellar lesion and bacteraemia. This was on the background of iatrogenic immunosuppression without recommended vaccination. The case highlights the importance of vaccinating immunosuppressed rheumatic disease patients.