19A122
PYODERMA GANGRENOSUM & LEUKOCYTOCLASTIC VASCULITIS AS A RARE COMPLICATION OF FLU VACCIANTION IN A PATIENT WITH PSORIATIC ARTHRITIS
Author(s)
Dr Sheraz Rasool, Dr Harsharan Kaur, Dr Denise De Lord.
Department(s)/Institutions
Department of Internal Medicine & Rheumatology, Queen Elizabeth the Queen Mother Hospital, East Kent University Hospital, Margate, Kent, UK.
Introduction
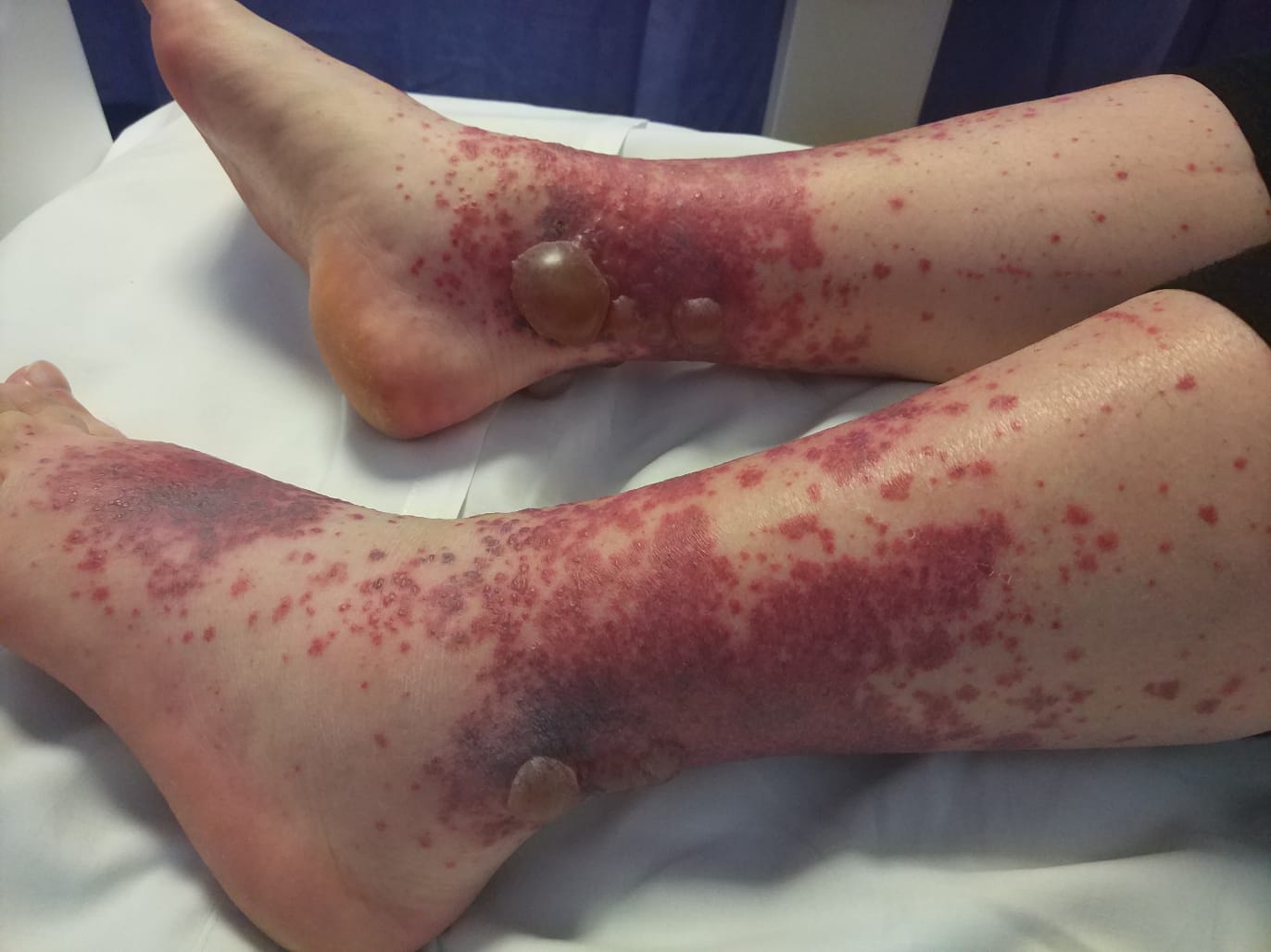
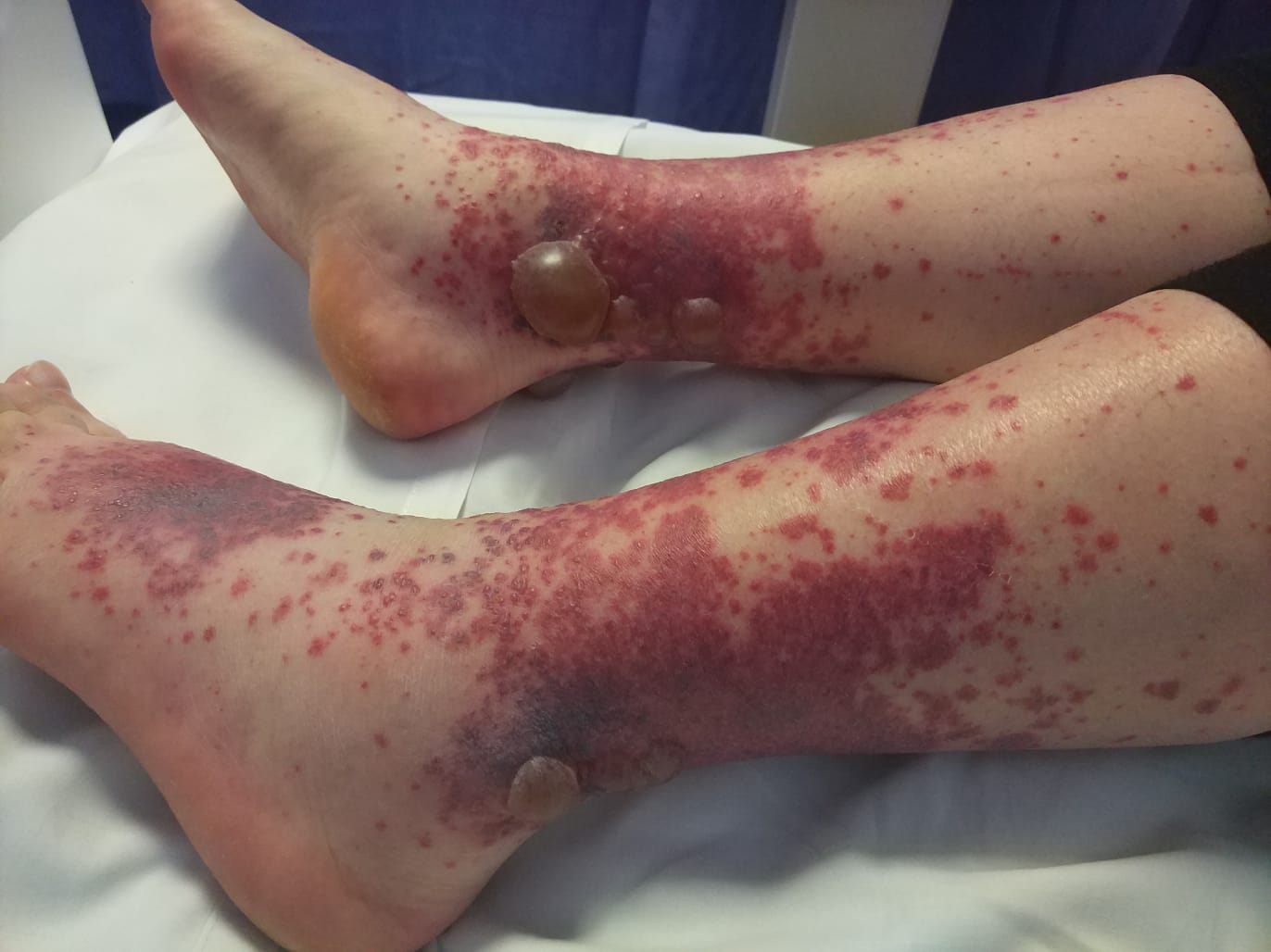
We report a rare complication of LCV and pyoderma gangrenosum in a patient with psoriatic
arthritis 5 days after immunization with a quadrivalent influenza vaccine. Humira and
methotrexate had been stopped several months earlier peri-operatively. The skin biopsy
confirmed the diagnosis of Leukocytoclastic vasculitis. Despite high dose intravenous and oral
steroids, the rash progressed with the development of Pyoderma Gangrenosum. Resolution of the
rash only occurred on re-starting immunosuppressive therapy.
Aims/Background
Leukocytoclastic vasculitis is categorized as small vessel vasculitis that presents with a skin rash
in form of palpable purpura mostly on the lower limbs. The most common triggering factors are
exposure to an infection or a new medication. In many cases, the cause is not identified. This is the first case report of the
development of LCV and Pyoderma gangrenosum post flu vaccination in a patient with psoriatic
arthritis. Early recognition of the association with the vaccination, rapid treatment and reinstitution
of immunosuppressive therapy resulted in rapid resolution of the cutaneous vasculitis
and PG.
Method
Although rare, LCV is a
recognized adverse effect following flu vaccination. Early diagnosis and treatment can prevent
prolonged hospital stay and morbidity. This is the first case report of the development of LCV
and Pyoderma gangrenosum post flu vaccination in a patient with psoriatic arthritis under 50
years of age. There is an increased risk of mortality secondary to influenza in those who are
immunocompromised. Temporary cessation of immunosuppressive therapy in this patient may
have precipitated the development of LCV and PG.
Results
The patient was treated aggressively with intravenous Methylprednisolone and later high dose
oral prednisolone. Methotrexate was re-started when infection was
excluded and then adalimumab on diagnosing pyoderma gangrenosum. The leucocytoclastic vasculitis responded to intravenous steroid but complete resolution of the
pyoderma gangrenosum only occurred on re-instituting adalimumab and Methotrexate. The rash
has now resolved completely with only residual scarring.
Conclusions
This is the first case report of the development of LCV and Pyoderma gangrenosum post flu
vaccination in a patient with psoriatic arthritis.
Caution should therefore be exercised in administering flu vaccines to patients who have
had their biological therapy temporarily discontinued.
Re administering flu vaccine to such patients should be carefully considered with
discussion with the patient of the pros and cons of flu vaccination, morbidity and mortality
of flu itself